Poster Presentation The Joint Annual Scientific Meetings of the Endocrine Society of Australia and the Society for Reproductive Biology 2017
Primary hyperparathyroidism in multiple endocrine neoplasia type 1: clinical significance and threshold for intervention (#224)
Context
Primary hyperparathyroidism (PHPT) is a common manifestation of multiple endocrine neoplasia type 1 (MEN 1). Hypercalcaemia due to parathyroid hyperplasia is manifest by the majority of gene carriers by age 30 years. Surgical management of hyperparathyroidism with extensive subtotal parathyroidectomy should occur when the risk of adverse clinical complications due to PHPT outweighs the risk of surgery, particularly the risk of hypoparathyroidism. However, it is unclear in MEN 1 as to when the benefits of surgery outweighs the risks.
Objective
To determine if there is an age related hypercalcaemic threshold for adverse sequelae in MEN 1.
Design, Setting, Participants
A single-centre retrospective observational study of peak serum calcium concentration and bone mineral density (BMD) in MEN 1 patients undergoing preoperative evaluation prior to parathyroidectomy.
Outcome Measures
Lumbar spine and femoral neck BMD measured by dual X-ray absorptiometry.
Results
Thirty one MEN 1 patients for whom BMD was assessed prior to parathyroidectomy were identified. Of these, 12 (38.7%) had evidence of mild hypercalaemia. Nineteen patients (61.3%) and 7 (22.6%) in aggregate met either osteopaenic and osteoporotic BMD criteria (Table).
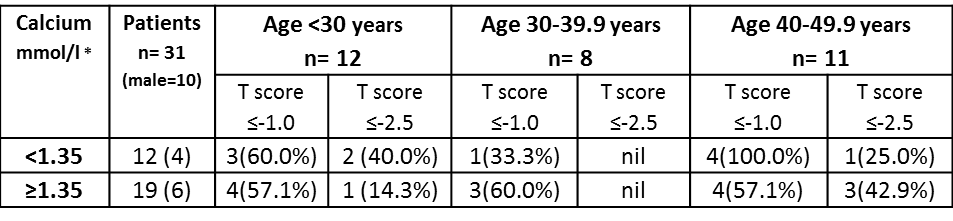
*Ionised Calcium or Corrected Calcium÷2
Conclusion
Our data indicate that skeletal complications are onset at both an early stage and age in MEN 1. We conclude that hypercalaemia alone is an unreliable indicator of potential biological impact of PHPT in MEN 1. Patients with even “mild” hypercalcaemia require consideration for treatment at an early disease stage.